Login to your account
- Private & confidential service
- Genuine medication
- All-inclusive service - No hidden fees
- Next day delivery
- Contraception
- Alternatives to the pill
- Evra Patch
Evra Patch
Buy Evra Patch after completing our online consultation for contraception
Prices include next-day delivery and prescription
| 3 months (9 patches) | £31.99 | |
| 6 months (18 patches) | £56.99 | Save £7 |
Select your treatment after the consultation:
More information about Evra Patch
What is the Evra Patch?
Evra is a convenient transdermal contraceptive patch used as a birth control method to prevent pregnancy and was introduced in the UK in 2002. Evra patch contains both artificial oestrogen and progestogen (norelgestromin and ethinylestradiol) and works in a very similar way to combined oral contraceptives (the pill) except that only one patch is required per week.
Also known as Ortho Evra, the patch releases a steady dose of hormones into your bloodstream through your skin, for the entire duration of your cycle. Similar to the vaginal contraceptive ring, it is easy to use and low maintenance contraception, providing an alternative for those who may be unable to take the traditional pill.
How does the Evra Patch work?
Ortho Evra's contraceptive hormones are released into the bloodstream through your skin and once they are in your system, they work in the same way as regular combination contraceptives. It prevents ovulation from occurring stopping the egg from being released when it is supposed to. This happens because the hormones in Evra patches, norelgestromin and ethinylestradiol, make the body think that ovulation has already happened.
As an additional measure, the transdermal birth control patch prevents sperm from entering the womb by changing the consistency of the cervical mucus and preventing the womb lining from thickening enough for an egg to attach and grow there.
The three-part process can be summarised as follows:
- It delivers a dose of oestrogen and progestogen, which prevents an egg from reaching the ovaries, thus stopping the ovulation
- Secondly, it thickens the cervix wall, making it more difficult for sperm to enter and reach the womb
- Thirdly, it thins the lining of the womb, stopping the egg, in the unlikely event of an egg getting released and fertilised, from implanting itself on the cervical wall
As with any birth control method, if you do not use the contraceptive patch in time or keep it on for too long, its effectiveness will be compromised. More information regarding this, and what you should do, is detailed below. The patch is also effective if you happen to vomit or have diarrhea as, unlike the contraceptive pill, it is absorbed straight into the skin. Please ensure you speak to your health care provider regarding the best method suited to you before using this hormonal contraceptive.
What are the benefits of Ortho-Evra?
The Evra contraceptive patch is a convenient alternative to the pill. The patch can be used every seven days to get complete protection. The patch also has some of the same benefits as the pill, such as:
- High contraceptive efficacy - more than 99% effective when used correctly
- Ease menstrual symptoms - can help to reduce irregular periods, menstrual cramps, or chance of endometriosis
- Low-maintenance - One patch is applied once a week, instead of taking one pill a day
- Easy to use - The patch is simply applied to a smooth area of the skin
- Non-invasive - Unlike a diaphragm or other similar methods, it doesn't need to be inserted into the vagina
- Minimal gastrointestinal side effects - Some women find taking a pill can upset their tummy (e.g. causing nausea and diarrhea). This is not the case with the contraceptive patch
- Can reduce the risk of other conditions - Including fibroids, ovarian cysts and breast disease (not associated with cancer)
How do I use the Evra Patch?
The patch is thin and beige in appearance at roughly 5cm x 5cm in size, working in the same way as a nicotine patch by releasing hormones into your bloodstream through the skin, rather than through ingestion.
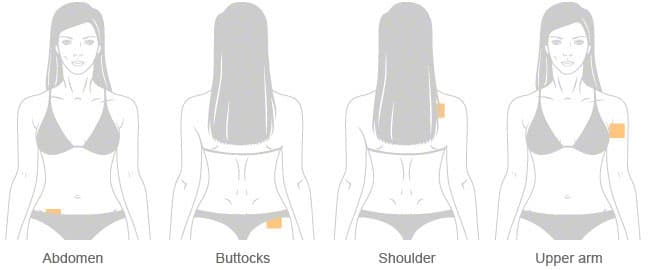 |
|||
| Abdomen | Buttocks | Shoulder | Upper arm |
Evra transdermal patches are used for three weeks (21 days) of your cycle, followed by a seven-day break period, during which you will still be completely protected. You should change your patch every seven days and apply a new patch on day eight. There are three patches in every 1-month supply box.
If you start using the patches within the first 24 hours of your period, you should be fully protected, but if you take use the patch later than that you should wait seven days before having sex or use an additional contraceptive method (such as the barrier method) .
- Apply the patch to clean, dry and smooth skin. Do not use any lotions or creams on that area
- The patch should stay on for 7 days. Check daily to make sure it is still in place.
- On the 8th day, remove 'Patch One' and apply the new patch immediately. You can change the location of each of your patches, remembering to always place on dry, clean and hair-free skin.
- 'Patch Two' stays on for the following 7 days. Check daily to make sure it is still in place.
- On the 15th day, remove 'Patch Two' and apply 'Patch Three' immediately. Again, you can change the location of the patch as desired.
- 'Patch Three' stays on for the remaining 7 days before the break period. Check daily to make sure it is still in place.
- On the 22nd day, remove 'Patch Three'. Do not apply another patch.
- The following seven days are your patch-free week and you may experience a withdrawal bleed similar to your period.
- Apply the next patch ('Patch One' from box 2) on the 29th day, regardless of whether you're still bleeding or not, and continue the cycle again.
As mentioned, the patch will be of immediate maximum effectiveness if applied within the first to fifth day of your period. Otherwise, use barrier protection or avoid sex for the next week.
What if I forget an Evra Patch?
There is not any research specific to the contraceptive patch concerning whether patients have forgotten to take off either patch one, two or three, or to apply a new patch after the 7-day break. However, the effects of the combined pill and the contraceptive ring can indicate the consequences as they work in a very similar way.
If I forget to apply the new patch after the 7-day break
- Up to nine days after the last patch (48 hours after the 7-day break) - you will still be protected providing you wore the previous three patches correctly. Apply your first patch of the month as soon as possible. This means your usual change dates have been altered slightly.
- If more than nine days have passed since taking off the last Evra patch - you will NOT be protected and will need to use additional barrier contraception for a further seven days. Your usual change dates are now altered but you should continue the three contraceptive patches as usual.
If you did not use further protection but had unprotected sex, you should consider getting the morning after pill. For further help on obtaining one of two emergency pills, head to our Morning After Pill page.
What to do if the patch falls off
The contraceptive patch is a sticky blighter that should stay in place securely throughout its seven days of use, even if exposed to humidity or situations which require extreme movement. This includes washing, swimming, exercising and other activities which may cause normal plasters to come off. However, should you experience any problems this is what you can do if it comes off:
Less than 48 hours - Stick your patch back on as soon as possible if it is still sticky. If it has lost its stickiness, throw away and apply a new patch. Do not try to salvage the damaged patch with plasters or tape, as this may decrease its effectiveness. Change to another new patch as initially scheduled.
More than 48 hours - You may not be protected against pregnancy during this period so you will need to use additional barrier protection (such as condoms) for seven days. However, you should still apply a new patch as soon as possible. This will alter your usual change dates.
What dosage is the Evra Patch?
There is only one dose of Evra, and it has been clinically tested. This means that you are effectively protected against pregnancy while posing minimal risk to your health. Ortho Evra has the active ingredients ethinylestradiol and norelgestromin. These are synthetic versions of the hormones estrogen and progesterone, respectively. The dosage levels for ethinylestradiol and norelgestromin are 203mcg and 34mcg, respectively. You can request a prescription for either a 3-month or 6-month supply at HealthExpress.
What are the possible side effects of the Evra Patch?
Some women experience side effects whilst applying the contraceptive patch. Like all contraception, side effects are rare and tend to be temporary, especially when starting a new medication. Common side effects that may be experienced when first using the treatment include:
- Headaches, breast tenderness, nausea, mood changes or light irregular bleeding
Rare sides effects of the contraceptive patch include:
- Vision or speech impairment, jaundice, breathlessness and chest pain
Contrary to popular belief, the patch will not make you gain weight, but you should be aware that the change in hormones may affect your eating habits negatively. If you do experience any adverse symptoms, you should always seek further medical advice from your GP.
It is also essential that you inform your doctor or health care provider before using the Evra patch, as research has shown it to slightly increase the risk of blood clots in women compared to the combined pill. For this reason, the FDA have provided a warning on the label to ensure those using it understand the risks and take the correct precautions.
What are the interactions/precautions to be aware of when using the Evra Patch?
For most women the Evra patch is a safe contraceptive, however, there are some scenarios that make it unsuitable. The Evra patch is contraindicated for women who are:
- Obese or morbidly obese
- Pregnant or breastfeeding
- Allergic to norelgestromin, ethinylestradiol or any other Evra ingredients
- Over the age of 35 (in particular smokers or recent ex-smokers)
- Smoking
- Diabetic
- Prone to severe migraines
In other cases women may need to exercise caution when applying the contraceptive patch. You should consult your doctor before starting treatment if you are at risk for or have experienced:
- Heart or circulatory problems (high blood pressure for example)
- Thrombosis (blood clots)
- Breast cancer (in the last five years)
- Severe migraines
- Liver or gallbladder disease
Although the Evra patch is generally well tolerated, caution is usually advised when taking it alongside certain other medications. Most antibiotics do not have an adverse reaction when used at the same time as the Evra patch, but some treatments may make Evra less effective. This includes:
- Epilepsy medication
- Amoxicillin
- Ritonavir
- Prednisone
- Topamax (topiramate)
- HIV or tuberculosis medication
- Levothyroxine
- St John's Wort
- Reserpine
It is always advised to visit your GP before starting a new form of contraception so that they can assess whether this contraceptive option is the best for you, or if an alternative may be more suitable.
Can I use the contraceptive patch during pregnancy and/or breastfeeding
If you think you could be pregnant, it is advised to stop using the contraceptive patch immediately. The patch is also not recommended if breastfeeding as it can reduce the amount of breast milk. Because of this, doctors seldom offer the contraceptive patch to new mothers before the 6-month mark.
How do I come off the patch or try to get pregnant after?
It is usually advised to wait until the cycle of the patch is complete, then you can stop using it at this point. You should be aware that your normal periods may not resume immediately and/or may take some months to regulate.
If you decide to remove the patch before the end of the cycle for reasons other than becoming pregnant, you increase the risk of an unwanted pregnancy, therefore it is essential that you tell your doctor before you do so. It is recommended that you use an alternative contraceptive method if you have decided against using the transdermal contraceptive patch.
If you are planning to have a baby, it is advised for you to wait for at least one standard period after stopping the use of the Evra patch before trying. This is to ensure that your body has reset to a normal cycle and that you can take the right steps towards pre- and mid-pregnancy care.
Dealing with unexpected pregnancy
If you accidentally have unprotected sex before using or after coming off Evra transdermal patch, you have the option of taking emergency contraception to prevent a pregnancy. This should be done as soon as possible after unprotected sex. The main options available are usually ellaOne (works within five days of intercourse) and Levonelle (works within three days of intercourse).
Please note: if you have already conceived/ are already pregnant, emergency contraception will not terminate this pregnancy but may cause harm to your child. Please seek advice with your doctor to determine your options in case of pregnancy.
Will the patch protect against STIs?
The only contraception that will protect you against STIs are barrier methods such as condoms, which are 98% effective when used correctly. Th contraceptive patch will protect against pregnancy, but not STIs (sexually transmitted infections).
How can I buy the Evra Patch online safely?
The contraceptive Evra patch is available from HealthExpress. You can order a 3-month or 6-month supply. To make sure the patch is safe for you, we need you to answer a few questions in your consultation. One of our registered doctors will make sure the patch is safe for you to buy and it can be dispatched for delivery within 24 hours.
| Product name | Evra |
| Active ingredient(s) | Ethinylestradiol and Norelgestromin |
| Manufacturer | Janssen-Cilag |
| Lowest price | £31.99 |
| Trustpilot rating | 4.7/5 |
| Trustpilot reviews | 108 |
| Availability | In stock |
| Description | Evra patch offers an effective alternative for those looking for contraception. It is proven to be 99% effective |
| Exemption | Subject to medical prescription |
| Administration | Topical |
| Presentation | Patches |
| Available dosage(s) | 203mcg/ 34mcg/ 24hrs |
| Application | Offering protection against pregnancy for women over 18 |
| Usage | Apply 1 patch every 7 days for 21 days followed by a 7 day break |
| Drug class | Combined patches |
| Alcohol consumption | No influence |
| Breastfeeding/pregnancy | Not recommended, ask your doctor for alternatives |
Note: Decisions about treatment are for both the prescriber and the person to jointly consider during the consultation. However, the final decision will always be the prescriber’s.
Evra Patch FAQs
The Evra patch is a highly effective contraceptive patch. It is over 99% effective at preventing pregnancy when taken correctly.
No, it is designed to allow for a withdrawal bleed during your patch-free week. On occasion, you may not have a bleed but if you have used the treatment correctly, you should still be protected. If you haven't had a withdrawal bleed and you're worried you have used the Evra patch incorrectly, you should take a pregnancy test.
Yes, acne is a common side effect of the Evra patch. If you're worried about your acne or any other side effects of the patch, you can head to our webpage about acne or consult your doctor.
Yes, Evra patches can cause weight gain in some women. However, weight gain may have many causes including variations during your menstrual cycle. If you're worried about side effects of the pill, please consult your doctor before taking it.
medical form
medication
prescription
from pharmacy
 Excellent
4.7
108 patients have reviewed Evra Patch on Trustpilot
Excellent
4.7
108 patients have reviewed Evra Patch on Trustpilot
It's easy to use
Nyangani NGood contraceptive- only have to remember once a week, is not visible, not many side effects, not affected by gut issues
B WGood price
Sihem SFurther reading

What are the benefits of taking contraception?
Reviewed by Dr. Anand Abbot

Your guide to hormonal contraception
Reviewed by Dr. Anand Abbot
Natural birth control: how does it work?
Reviewed by Dr. Anand Abbot
What you should know about permanent contraception
Reviewed by Dr. Anand Abbot
The IUD and IUS Contraceptive Guide
Reviewed by Dr. Anand Abbot
Your guide to barrier methods of contraception
Reviewed by Dr. Anand Abbot- Helpful and friendly customer serviceWe’re available Mon - Fri, 08:00 - 17:00
- No hidden feesAll prices include shipping & prescription
- Next-day deliveryFor all orders before 16:30



